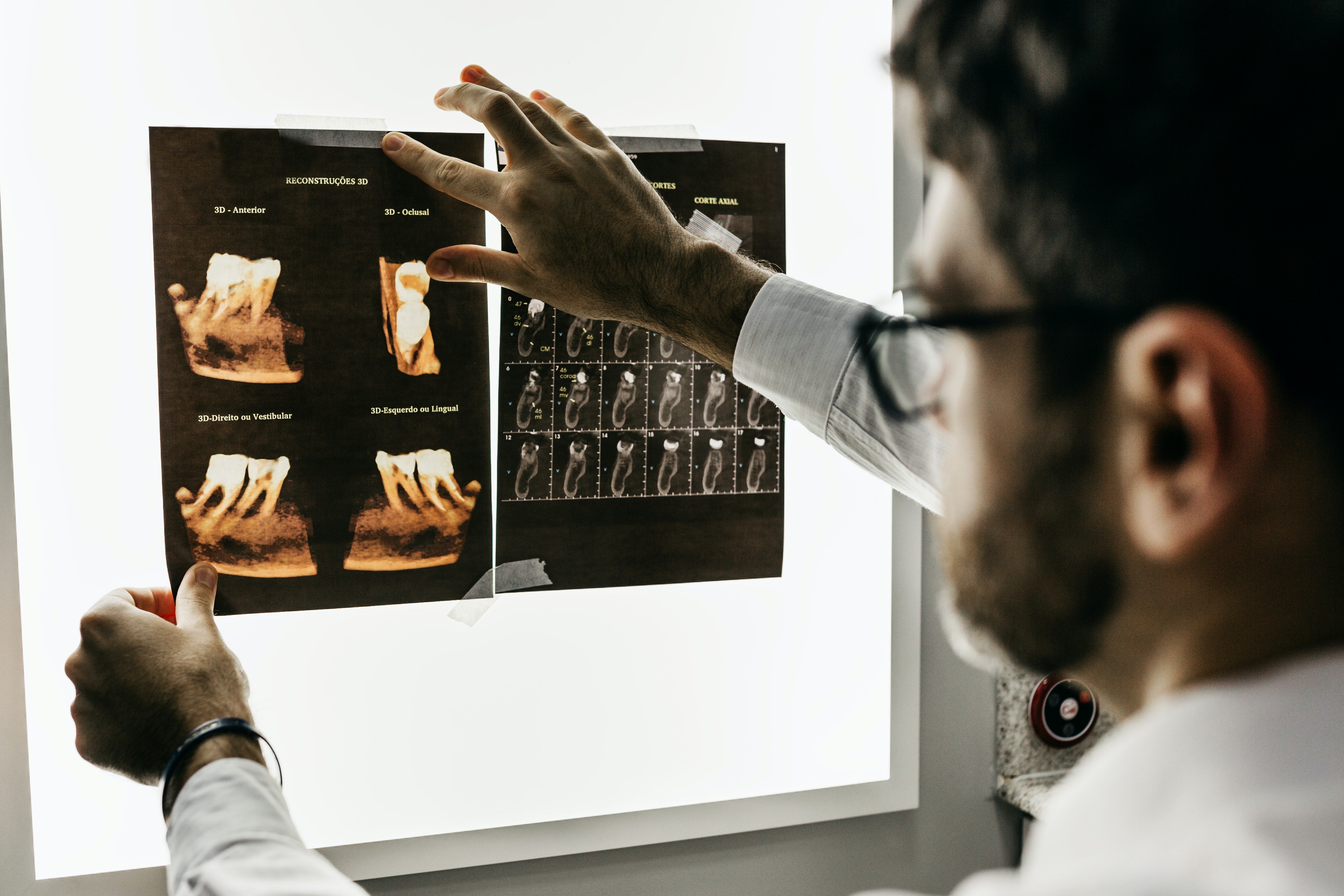
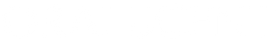Systemic Diseases Linked to Gum Disease
Cardiovascular Diseases – Bacterial plaque from the oral cavity can make its way into a person’s bloodstream through the open area of infection and blood flow just under the gumlines. The plaque then travels through the arterial system and can become lodged in arterial plaque or find its way into the heart. People that have suffered from heart attacks and strokes have been found to have oral bacteria present in the area where the blockage or attack took place.
Diabetes – Managing blood sugar levels is almost impossible when there is active gum disease. Likewise, bacteria feed on sugar, so when blood sugar levels are elevated, gum disease becomes advanced and unmanageable. The two conditions go hand-in-hand. Managing oral plaque through good daily hygiene and controlling blood sugar levels through nutritional restrictions are essential. Diabetics must take their oral health seriously if they wish to extend the lifetime of their smile.
Erectile Dysfunction – Clinical studies show that there is a correlation between chronic periodontal disease and the management of erectile dysfunction. This is thought to be due to the damage of internal epithelial tissue during an inflammatory response of the body. The same studies suggest that managing periodontal disease is an effective preventive measure to manage or prevent erectile dysfunction.
Obesity – Gum inflammation and periodontal disease may be linked to adults and children who are obese. Studies show that obesity may also cause advanced loss of bone around the teeth. The theories around obesity causing gum disease differ, and the relationship may also involve some aspects of blood sugar levels, such as in patients with diabetes. Regardless of whether or not it causes the induction of gum disease, obesity is considered a significant risk factor for periodontal diseases.
Premature Labor and Infants of Low Birth Weight – Oral bacteria can enter the placenta the same way it enters into the cardiovascular system, which is through areas in the mouth that have active gum disease. Pregnant women with active periodontal disease symptoms are shown to have an increased risk of going into labor prematurely. Babies born to these women are also likely to have low birth weights, even if they are born closer to full term.
Symptoms of Oral Infections when Systemic Diseases are Present
When someone is actively battling a systemic health condition, his or her oral health is typically diminished from what it should be. Only when the condition is truly managed will the person possibly expect to have healthy gum tissues. Gingiva in a person with a compromised immune system may exhibit a combination of the following symptoms:
- Bleeding gums – Elevated immune responses in the body send antibodies throughout the bloodstream to areas that are infected with bacterial infections. One of these areas is the gumlines in people with gingivitis or periodontal disease. It can be more difficult to gain control over bleeding, even when oral hygiene practices are adequate.
- Gum recession – Loss of tissue attachment in areas of oral infection can cause the gums to recede, making teeth appear longer and exposing sensitive root surfaces.
- Swelling or excessive growth of gum tissue – Inflammation of the gingiva may occur more frequently and be more difficult to manage when the body is strained by other coexisting conditions. Excess tissue growth may also be a side effect of medications taken for conditions like high blood pressure. While this fibrous tissue growth is not problematic, it can be unsightly and make oral hygiene more difficult.
- Bone loss – Degenerative bone diseases may predispose a person to bone loss in the jaw. Also, when advanced gum disease is difficult to manage due to poor health, unmanageable bacterial levels will result in bone loss around the teeth. Tooth mobility and loss are imminent when bone loss is severe.
- Pale gingiva – If anemia is present, gum tissue may lose its coral color and become pale in appearance, due to lack of red blood cells in the tissues.
Risk Factors
Understanding the risk factors associated with your specific health condition allows you to be better aware of whether or not you are managing it effectively. The fact is that having a systemic health disease will in and of itself be a risk factor in developing gum infections like periodontal disease or other oral health problems.
A person’s risk factors will be directly linked to the conditions, symptoms, and current health status of the disease that they are attempting to manage, as those are the factors that will strain the body’s immune system as it attempts to help heal other coexisting infections.
Gum infections are a risk factor for your systemic health
As mentioned above, having uncontrolled gum infections like periodontal disease are directly linked with the severity of systemic health problems. If a person does not attempt to manage the health of their gums, then they are increasing their likelihood of suffering complications associated with other health problems, even if an attempt is made to manage them.
Treating gum disease in a person that has an active systemic disease condition can be extremely difficult. Due to the strain on the immune system from other health conditions, the body may not be able to fully fight off the effects of bacterial plaque in the mouth, allowing it to advance into a more severe disease state. Gaining control over gum disease can only be truly achieved when both the gum infection and the systemic conditions are addressed together.
Follow your primary care physician’s recommendations to manage or cure your systemic health problem
Obviously, for some types of conditions it isn’t always possible to completely cure yourself. However, most conditions like obesity or diabetes, for example, require adhering to a strict diet and participating in regular exercise. If you decide you don’t want to even try developing healthier habits, then you’re not going to see improvement in those conditions or any of your others. See your care provider on a regular basis and take their recommendations to heart.
Take medication as directed
Eliminating medication without advising your doctor may cause serious side effects. Some people space out medication due to convenience or budget, but that can allow rapid irregularities to occur, increasing the likelihood of complications or medical emergencies. Wean yourself from medications only as your physician sees that you can manage your condition in other ways such as diet and exercise. In the ideal situation, a person and their doctor can come up with a way to get off of some medications when healthy lifestyle choices become a normal part of everyday life.
See your dentist for routine preventive or therapeutic care
Whether you need cleanings every 6 months, or gum disease treatments like deep cleanings, it’s important to see your dentist and hygienist regularly. Neglecting professional care when you have active systemic disease conditions can allow gum disease to progress very rapidly. Patients with a history of moderate to severe periodontitis may need to be seen as often as every 3 or 4 months for preventive cleanings.
Practice the best daily oral hygiene possible
If you have health problems, you have more of a reason to practice exceptional oral hygiene than other people. Brush twice each day for at least 2 minutes or longer, with the toothbrush angled toward the gumlines. Utilize blue light technology to effectively reverse gum disease including gingivitis, bleeding, swollen, and receding gums.
Floss
Floss or use another type of interproximal cleaning device (such as a water flosser) at least once per day to remove bacteria from under the gums that have the potential to be transmitted to the bloodstream. Mouthwash is not regarded as an effective oral hygiene aid, as it does not physically remove plaque from the surface of the teeth or below the gumlines. Instead it can be used after brushing and flossing to aid in antibacterial actions, freshen breath, and deliver fluoride to the enamel as needed.